 .
.
.
.
.
Part Two : 2011 HCV and Wall Street
...
Jan 20th/Telaprevir
.
Updated: Jan 6th/Boceprevir
...., ..,
Week Of Feb 7th
.
If a lot of chemistry work has to be done later and what we put in development is not the original compound, then we take the IP in case the same molecule can be used in a commercial environment. For example, some compounds for dengue might also work for Hepatitis C, which is a blockbuster. We could give that IP to Novartis’ pharmaceutical department, which is a commercial organization.
..
Idenix Pharmaceuticals to Present at Two Upcoming Investor Conferences
Written by TradersHuddle Staff Monday, 07 February 2011 16:08
CAMBRIDGE, Mass.-( Business Wire )-
Idenix Pharmaceuticals, Inc. (NASDAQ: IDIX), announced today that Idenix management will present a corporate overview at the 13th Annual BIO CEO & Investor Conference on February 14, 2011 at 10:30 a.m. ET at the Waldorf Astoria, New York City and at the Leerink Swann Hot Topics Roundtable Conference on February 16, 2011 at 2:20 p.m. ET at the Roosevelt Hotel, New York City. The live and archived webcasts of the company presentations can be accessed under “Calendar of Events” in the Idenix Investor Center at www.idenix.com. Please log in approximately 5-10 minutes before each event to ensure a timely connection. The archived replay will be available on the Idenix website for two weeks following the conferences. .
Week Of Feb 1st
.,,.
The fourth quarter net loss was $531 million, or 17 cents a share, the Whitehouse Station, New Jersey-based company said. The company withdrew its long-term profit forecast of high single-digit growth through 2013. In the past quarter, Merck's hepatitis C drug, boceprevir, won expedited reviews by regulators in the U.S. and European Union. A decision by the U.S. Food and Drug Administration is also expected this year on an extended version of the Janumet diabetes pill, which combines Merck's Januvia with a generic drug called metformin. ,
Vertex Loses $180M in Q4Vertex Pharmaceuticals Inc. reported a larger fourth-quarter loss as it spent more money to develop its hepatitis C drug candidate telaprevir, along with a potential cystic fibrosis treatment and other drugs. ...continue ..
2/2/11
If Vertex Pharmaceuticals gets its way in talks with U.S. public health officials, most people over 50 could soon get blood tests to screen for hepatitis C infections at the doctor’s office. If the U.S. Centers for Disease Control and Prevention (CDC) agrees this is a good idea, it could prompt another 1 million patients who don’t realize they are infected to come out of the woodwork and start clamoring for Vertex’s new hepatitis C drug over the next few years./0.5/11
Idenix Pharmaceuticals to Present at the 29th Annual J.P. Morgan Healthcare Conference .
Vertex Pharmaceuticals Incorporated (Vertex) is engaged in the business of discovering, developing and commercializing small molecule drugs for the treatment of serious diseases. Telaprevir, the Company’s lead drug candidate, is an oral hepatitis C protease inhibitor and a new class of antiviral treatments in clinical development that target hepatitis C virus (HCV), infection. Telaprevir is being evaluated in a registration program focused on treatment-naïve and treatment-failure patients with genotype 1 HCV infection. VX-770, the lead drug candidate in its cystic fibrosis (CF), program is being evaluated in a registration program that focuses on patients with CF who have the G551D mutation in the gene responsible for CF. Vertex is conducting a number of Phase IIa clinical trials of its earlier-stage drug candidates. On March 12, 2009, Vertex acquired ViroChem Pharma Inc. (ViroChem)
..
,..
Bayer teams up in India
German pharma and chemical group Bayer and Indian company Zydus Cadila have agreed to create a new company in India called Bayer Zydus Pharma. Each company will have a 50 per cent stake in the joint venture and equal representation on the management board. Bayer says it is looking to strengthen its position in the Indian pharma market. About 600 employees will transfer to the new company from the parent companies.
. Teva buys Peruvian generics firm
Israeli generics firm Teva has said it will buy Corporacion Infarmasa, a pharmaceutical company based in Peru, from the two investment companies that own it. Teva already owns a company based in Peru: Corporacion Medco. Infarmasa makes generics, including corticosteroids, antihistamines, analgesics and antibiotics, at two sites in Lima. Financial details were not disclosed. ,
Arena Pharmaceuticals: Should The CEO Go?
By Ed Silverman // January 31st, 2011 // 10:37 am
For the past few months, Arena Pharmaceuticals ceo Jack Lief has been at the center of controversy over the extent to which the drugmaker’s Lorqess diet pill may have links to tumors in rats and, more specifically, whether data about this possibility was disclosed correctly. Last September, he was chastised for not conveying any info prior to disclosure that was made publicly by FDA staffers, who discussed the data in documents submitted for an FDA advisory panel .
For example, consider just a few companies with new breakthrough drugs that are expected to become blockbusters (among nearly a dozen others): Dendreon’s (Nasdaq: DNDN ) prostate cancer drug, Provenge. Vertex Pharmaceuticals’ (Nasdaq: VRTX ) hepatitis therapy, Telaprevir. The drug is expected to receive FDA approval in May and could generate as much as $4 billion in annual sales. Human Genome Sciences’ (Nasdaq: HGSI ) treatment for lupus.
But these “hotshot” analysts are also overlooking what I think will be the biggest growth area for biotech in the coming months…
.
Week Of Jan 24
J&J Disappoints, 2011 Outlook Weak
Johnson & Johnson's (
JNJ -
Analyst Report) fourth-quarter 2010 earnings (excluding special items) of $1.03 per share was in-line with the Zacks Consensus Estimate and a penny above the year-ago earnings of $1.02. Full year earnings came in at $4.76 per share, a penny above the Zacks Consensus Estimate and 2.8% above the year-ago earnings.
,,
Drugmaker Vertex moving to Fan PierCambridge-based Vertex Pharmaceuticals has signed a non-binding letter of intent for two buildings on Fan Pier, the company said.Under the terms of the deal, developer Joseph Fallon would build 1 million square feet of office and research and development space on the waterfront. Signing the lease would be contingent on Food and Drug Administration approval of Vertex’s drug to treat hepatitis C, according to Vertex spokesman Zachry Barber...
read more ,
PRINCETON, N.J., Jan. 24, 2011 /PRNewswire/ -- Pharmasset, Inc. (Nasdaq:
VRUS) announced today the underwriters of its recent underwritten public offering have exercised their option to purchase from Pharmasset an additional 495,000 shares of common stock.
,,
Week Of Jan 17th
m,..
May is going to be a solid month for drug approvals.The multiyear marathon between Schering-Plough and Vertex Pharmaceuticals (Nasdaq: VRTX) to develop the next-generation hepatitis C drug is finally coming to a close. Vertex announced yesterday that the Food and Drug Administration has accepted its New Drug Application to market telaprevir. Not surprisingly, given the unmet need, the agency will give telaprevir a priority review, so Vertex should hear back on or before May 23.Merck (NYSE: MRK), which took over development of boceprevir when it bought Schering-Plough, announced a few weeks ago that the FDA had accepted its application with a priority review, as well. Since one drug isn't all that material to Merck's business, the company didn't feel compelled to give an exact date of the submission, so we don't know exactly when the FDA will come back with a decision. ,.
Bristol-Myers Squibb touted the five drugs in its pipeline that could reach the market by 2012; Pfizer highlighted its four most advanced oncology drugs; Merck & Co. emphasized its deep investment in cardiovascular drugs and the speedy filing of a New Drug Application for the hepatitis C drug boceprevir .
have teamed up in a clinical partnership that marks the first cross-company collaboration to study two investigational oral drugs for the treatment of hepatitis C. The firms announced plans to study Bristol's NS5A replication complex inhibitor BMS-790052 and Pharmasset's nucleotide polymerase inhibitor on Jan. 10.
Drug makers do not generally collaborate on clinical trials for investigative drugs for competitive reasons and tend instead to study combinations within their own pipelines or with at least one already marketed drug. Regulatory uncertainties and, perhaps, just as important, cultural resistance, also present hurdles. But novel-novel combinations increasingly are viewed as the best way to treat certain serious diseases, like cancer and hepatitis C, and have become more common.
In hepatitis C specifically, the primary drug development focus is on combinations that could replace or reduce the use of the current standard of care, ribavirin and pegylated interferon (Roche's Pegasys or Merck's Pegintron), a regimen with a hasty side effect profile and limited efficacy. Bristol's decision to sign a clinical trial collaboration rather than in-licensing a polymerase inhibitor is intersting since the company recently acquired its hepatitsi C partner ZymoGenetics to gain more control over the program.
,
....,
After the recalls of tens of millions of bottles and packages of numerous over-the-counter meds and surgical devices; months of negative publicity about corporate behavior; various government investigations and highly publicized congressional hearings, consumers may be turning away from Johnson & Johnson (
JNJ) OTC products (back stories
here,
here,
here and
here).
In the last quarter of 2010, Johnson & Johnson’s share of the $4.2 billion cough and cold market sank to about 5 percent from about 17 percent in early 2009, according to Nielsen data cited by Wells Fargo analyst Larry Biegelsen in an investor note. The J&J share of the $2.4 billion pain and arthritis market fell to just below 10 percent from just under 20 percent during the same period, while its share of the $1.4 billion gastrointestinal market slid to less than 5 percent from more than 10 percent.
...
Sunday, January 16, 2011
Merck/Parexel International: Merck was one of the first companies to announce a strategy for bringing low-cost biologic copies to market after U.S. healthcare reform provided a clearer regulatory path for biosimilars. It announced the formation of a BioVentures unit in December 2008, with plans to put at least six biosimilars in development by 2012. It has kept close to the vest details of its target priorities, however, noting publicly only its interest in Amgen's granulocyte colony-stimulating factors Neupogen (filgrastim) and Neulasta (pegfilgrastim).
Now, the Big Pharma has struck a partnership with clinical research organization Parexel International Corp. in which the CRO will conduct clinical trials for some of Merck's biosimilar programs. True to form, the companies won't say which therapeutic areas are covered by their collaboration, however. "One of the things that was exciting for us is that we were able to build a deal structure with Parexel in which they are rewarded for performance," Merck BioVentures President Michael Kamarck told "The Pink Sheet" DAILY. "In the biosimilars arena, time is everything, so...they will rpovide us with timeliness, and efficiency in execution of trials." -- Lisa LaMotta.
.
Week Of Jan 10th
.,.,.
India is moving toward an innovative culture that will drive biotechnology’s continued growth. We are moving in the right direction – the Indian biotechnology sector’s prospects have never looked brighter. But there is more work that needs to be done. We need to increase collaborations and deal making across the biotech industry in India and globally, while promoting our assets and capabilities to global biotechnology and pharmaceutical companies as well as to investors and other financial stakeholders. Many biopharmaceutical companies want to diversify into generic drugs and biosimilars and are looking to India for partners based on our leadership in those segments.
,
Biosimilars: Empty Threats?The
Jan. 10 announcement by Novartis' Sandoz division of the start of Phase II trials of a biosimilar version of Roche's rituximab (Rituxan) is beginning to look a bit like posturing. After all, when was the last time a biosimilars firm gave away anything about its pipeline, let alone details of a specific compound?
,,
By Deena Beasley
SAN FRANCISCO Thu Jan 13, 2011 3:57pm EST
SAN FRANCISCO (Reuters) - More drugmakers are seeing potential in the business of producing copycat versions of expensive biotechnology drugs as U.S. guidelines take shape.
The topic was at the forefront of plans discussed by several executives at this week's JP Morgan healthcare conference in San Francisco.
Kevin Sharer, chief executive officer at Amgen Inc, said the world's largest maker of branded biotechnology drugs would consider entering the "biosimilars" space, particularly in emerging markets like Asia and South America.
..
Should Merck Have Bought Schering-Plough?
The merger has always been about much more than any one product. This merger was about taking two strong companies and making an even stronger one. As a result of the merger, the combined company is much better positioned to address the evolving needs of today’s healthcare environment:
-Strong late-stage pipeline with boceprevir, odanacatib and anacetrapib, among others. [Matt adds: those are for hepatitis C, osteoporosis, and heart disease]
.,
,
By Thomas Gryta Of DOW JONES NEWSWIRES
NEW YORK (Dow Jones)--Vertex Pharmaceuticals Inc. (VRTX) Chief Executive Matthew Emmens is ready to go toe-to-toe with one of the world's biggest pharmaceutical companies, Merck & Co. (MRK).
Cambridge, Mass., based Vertex has filed for Food and Drug Administration approval of telaprevir, which has shown a sharp increase in cure rates of hepatitis C in multiple studies when added to current treatments. Merck also has shown success with its similar drug, boceprevir, and has filed for approval with expedited review granted in both the U.S. and Europe.
The drugs are expected to come to the market at similar times and create a market share battle, but Emmens isn't concerned about the size mismatch.
.,
In its first move into the potentially lucrative Chinese market, Ligand Pharmaceuticals said Thursday that it partnered with the U.S. affiliate of a Hong Kong drug company to develop and market two experimental liver disease drugs in China.
.
Jan 11, 2011 (Datamonitor via COMTEX) --
Bristol-Myers Squibb Company and Pharmasset have entered into a clinical collaboration agreement to evaluate the utility of BMS-790052, Bristol-Myers Squibb's NS5A replication complex inhibitor, in combination with PSI-7977, Pharmasset's nucleotide polymerase inhibitor, for the treatment of chronic hepatitis C virus, or HCV.
This proof of concept study will evaluate the potential to achieve sustained viral response 24 weeks post treatment with an oral, once-daily treatment regimen in patients
across HCV genotypes.
.
(NASDAQ:VRTX) percentage change grew 0.36%, to close at $36.29 and its overall traded volume was 2.16M shares on Monday, the stock had average daily volume of 1.72M shares. VRTX opened at $35.95 and is trading within the range of $35.71-$36.54. The 52-week range of the stock is $31.25 – $43.94. The market capitalization of the company stands at $7.37B and it has 203.19M outstanding shares.Vertex Pharmaceuticals Incorporated (Vertex) is engaged in the business of discovering, developing and commercializing small molecule drugs for the treatment of serious diseases. Telaprevir, the Company’s lead drug candidate, is an oral hepatitis C protease inhibitor and a new class of antiviral treatments in clinical development that target hepatitis C virus (HCV), infection. Telaprevir is being evaluated in a registration program focused on treatment-naïve and treatment-failure patients with genotype 1 HCV infection. VX-770, the lead drug candidate in its cystic fibrosis (CF), program is being evaluated in a registration program that focuses on patients with CF who have the G551D mutation in the gene responsible for CF. Vertex is conducting a number of Phase IIa clinical trials of its earlier-stage drug candidates. On March 12, 2009, Vertex acquired ViroChem Pharma Inc. (ViroChem).,
..
On November 22, 2010, Vertex completed the submission of its New Drug Application (NDA) for telaprevir to the United States Food and Drug Administration (FDA). A response from the FDA regarding the company’s request for Priority Review of the telaprevir NDA is expected this month. The FDA’s goal for completion of its review for NDA submissions granted Priority Review status is six months from the NDA submission date
..
(BUSINESS WIRE) -- ---Cystic Fibrosis: First Phase 3 data for VX-770 expected in first quarter 2011- ---Additional ongoing trials in HCV, CF, epilepsy and rheumatoid arthritis- ---Vertex enters 2011 with cash and cash equivalents position of more than $1 billion- Vertex Pharmaceuticals Incorporated (NASDAQ: VRTX) today announced its 2011 business objectives in conjunction with the 29th Annual J.P. Morgan Healthcare Conference in San Francisco. Matthew Emmens, Chairman, President and Chief Executive Officer of Vertex, will discuss these objectives as part of a live webcast presentation, which will be available on Vertex's website,
http://www.vrtx.com/ , on Monday, January 10 at 9:30 a.m. PT (12:30 p.m. ET).
"2011 will be a landmark year for Vertex as we prepare for the expected launch of telaprevir in hepatitis C and advance other new therapies in development," said Mr. Emmens.
.,,
Chiva Pharmaceuticals in-licensed China rights for two clinical-stage liver drugs from Ligand Pharma (NSDQ:
LGND) (see
story). It also will receive non-exclusive rights to Ligand’s HepDirect technology to discover and develop new molecules for hepatitis B, hepatitis C and hepatocellular carcinoma. Chiva, which is headquartered in California, is an affiliate of Hainan Kaihua Pharma.
.
January 2011 00:20
Inhibitex, Inc. today reported positive preliminary interim safety and antiviral data from the first two monotherapy cohorts of its ongoing Phase 1b clinical trial of INX-189, an oral NS5b nucleotide inhibitor being developed to treat chronic infections caused by
hepatitis C virus (HCV).
..,
Week Of Jan 3rd
.
The U.S. Food and Drug Administration accepted Merck's approval filing for its hepatitis C drug boceprevir, the company said Thursday. The news from Merck is a bit of a surprise since the company hadn't previously announced or confirmed that boceprevir had been filed with U.S. regulators. It's also a tad embarrassing for Vertex, which is still waiting to hear back from FDA about the acceptance of the approval filing for telaprevir, its
competing hepatitis C drug. That news should come by Jan. 24, based on Vertex's previous announcement that it filed the drug's application on Nov. 23. Still, it seems as if Merck beat Vertex to the FDA by at least two weeks.
Continue Reading.... ,
Pharmasset Reports Positive Results from its HCV Clinical Programs - PSI-7977 400mg QD with pegylated interferon and ribavirin was generally safe and well tolerated while demonstrating potent viral suppression in patients with HCV genotype 2 or 3 over 12 weeks of dosing- PSI-938 300mg QD monotherapy was generally safe and well tolerated over 14 days of dosing and demonstrated potent antiviral activity and no viral breakthrough
.
BASi (Bioanalytical Systems Inc.), a life sciences company in the Purdue Research Park, has entered into a Preferred Provider Agreement (PPA) with Princeton, New Jersey-based Pharmasset Inc., a clinical-stage pharmaceutical company committed to discovering, developing and commercializing novel drugs to treat viral infections, to provide preclinical services for pre-IND and post-IND activities. The agreement includes provisions to provide exclusive toxicology services as well as pharmaceutical analysis and bioanalytical services as needed.
.
Chiva Pharmaceuticals negotiated Chinese development rights to
Ligand Pharmaceuticals’ clinical-stage
HepDirect candidates,
Pradefovir for hepatitis B (hepB) and
MB01733 for
hepatocellular carcinoma (HCC). The deal also gives Chiva a nonexclusive license to use Ligand’s HepDirect technology for the discovery, development, and worldwide commercialization of new candidates against hep B, hep C, and HCC.
Pradefovir is a HepDirect prodrug of PMEA, the active metabolite in the FDA-approved HepB drug adefovir dipivoxil (Hepsera®). The drug is currently in Phase II development in the U.S. MB07133 is a HepDirect prodrug of the intermediate form of cytarabine (araC) 5’-monophosphate. Currently in Phase I/II development treatment of hepatocellular carcinoma, the drug has already demonstrated strong response rates in terms of intrahepatic tumor regression in a U.S. trial, Ligand states.
.
.
Piper Jaffray Overweight On Vertex Pharmaceuticals (VRTX)
By
Jonathan Chen Benzinga Staff WriterJanuary 06, 2011 8:01 AM
...
.
The supply of the Hepatitis C drug to Vertex by Shasun Chemicals is set to take off earlier than anticipated. The product is set to launch in June-July next year. "Commercial supplies have already started and we are preparing for the launch this year," says Vimal Kumar, Managing Director of Shasun Chemicals, in an exclusive interview with CNBC-TV18's Udayan Mukherjee and Mitali Mukherjee. ..
Pharmasset to Present at the 29th Annual J.P. Morgan Healthcare Conference
,
PRINCETON, N.J., Jan. 4, 2011 /PRNewswire/ -- Pharmasset, Inc. (Nasdaq: VRUS) announces that management will present at the 29th Annual J.P. Morgan Healthcare Conference to be held January 10-13, 2011 at the Westin St. Francis Hotel, San Francisco, CA. Schaefer Price, President and Chief Executive Officer, will provide an overview of the company on Wednesday, January 12, 2011 at 9:00 AM (PT).
To access a simultaneous webcast of Mr. Price's overview via the internet, log on to the "Events & Presentations" section of the Investor Center on Pharmasset's website at http://investor.pharmasset.com/events.cfm. Please connect to the website at least ten minutes prior to the start of the presentation to ensure adequate time for a reliable connection and any software download that may be necessary for the webcast.
A replay of the webcast will be available on Pharmasset's website for thirty days following the conference. The investor presentation will be available for download in PDF format immediately following the presentation in the "Events & Presentations" section of the Investor Center on Pharmasset's website at http://investor.pharmasset.com/events.cfm. .,
After the bell Tuesday, Anadys Pharmaceuticals, Inc. (Nasdaq:ANDS) announced that it has initiated the planned Phase IIb study of ANA598 in combination with pegylated interferon and ribavirin. The protocol for the study has been cleared by the United States Food and Drug Administration and Health Canada. Patient screening has begun and patient dosing is expected to commence within the next several weeks. In the study ANA598 will be tested in both treatment-naive patients and treatment-experienced patients who failed a prior course of therapy with interferon and ribavirin. ANA598 is the Company's direct-acting antiviral, or DAA, being developed for the treatment of hepatitis C.Earlier Tuesday: Shares of XOMA Ltd. (Nasdaq:XOMA) have caught fire once again. Today the company announced a partnership with Les Laboratoires Servier (Servier), France's largest privately-held pharmaceutical company, to develop and commercialize XOMA 052, XOMA's anti-inflammatory drug candidate, in multiple indications. The drug is designed to inhibit the pro-inflammatory cytokine interleukin-1 beta that is believed to be a primary trigger of pathologic inflammation in multiple diseases.
,
From Tape Beat
InterMune, Inc. (NASDAQ:ITMN) decreased -0.34%, currently trading at $37.78 and its overall traded volume was 1.04M shares while reporting, against its average volume of 2.44M. ITMN opened the day at $37.64, it made an intraday low of $36.98 and an intraday high of $38.58. The stock has a 52 week low of $8.34 and 52 week high of $49.46. ITMN's market capitalization is 2.12B and it has 56.03M outstanding shares. InterMune, Inc. (InterMune) is a biotech company focused on developing and commercializing therapies in pulmonology and hepatology. In November 2008, InterMune together with Roche and Pharmasset, Inc. (Pharmasset) announced the initiation of INFORM-1, a dual combination clinical trial investigating the combination of two oral antiviral molecules in the absence of interferon. In August 2009, the Company together with Hoffmann-LaRoche Inc. and F. Hoffmann-LaRoche Ltd. (collectively Roche) began a Phase IIb study testing RG7227 in combination with PEGASYS (peginterferon alfa-2a) and COPEGUS (ribavirin), the standard of care (SOC) in hepatitis C virus (HCV).
..
.
Vertex Pharmaceuticals Incorporated (Vertex) is engaged in the business of discovering, developing and commercializing small molecule drugs for the treatment of serious diseases. Telaprevir, the Company’s lead drug candidate, is an oral hepatitis C protease inhibitor and a new class of antiviral treatments in clinical development that target hepatitis C virus (HCV), infection. Telaprevir is being evaluated in a registration program focused on treatment-naïve and treatment-failure patients with genotype 1 HCV infection. VX-770, the lead drug candidate in its cystic fibrosis (CF), program is being evaluated in a registration program that focuses on patients with CF who have the G551D mutation in the gene responsible for CF. Vertex is conducting a number of Phase IIa clinical trials of its earlier-stage drug candidates. On March 12, 2009, Vertex acquired ViroChem Pharma Inc. (ViroChem).
Shares of Vertex Pharmaceuticals (NASDAQ: VRTX) traded down 0.79% during mid-day trading on Friday, hitting $35.06. Vertex Pharmaceuticals has a 52 week low of $31.25 and a 52 week high of $44.24. The stock’s 50-day moving average is $34.28 and its 200-day moving average is $34.94. On average, analysts predict that Vertex Pharmaceuticals will post $-0.90 EPS next quarter. The company has a market cap of $7.124 billion and a price-to-earnings ratio of N/A.
For more information about
Zacks Investment Research’s equity research offerings, visit
Zacks.com.
.
.
Zacks Investment Research research analysts reiterated a “neutral” rating for shares of Achillion Pharmaceuticals Inc (NASDAQ: ACHN) in a research note issued to investors on Thursday.
Achillion Pharmaceuticals Inc (NASDAQ: ACHN)’s stock traded down 1.20% on Monday, hitting $4.10. Achillion Pharmaceuticals Inc has a 52 week range of $1.99 to $4.20. The stock’s 50-day moving average is $3.1 and its 200-day moving average is $2.77. Analysts predict on average that Achillion Pharmaceuticals Inc will post $-0.13 earnings per share next quarter. The company has a market cap of $239.2 million and a P/E (price-to-earnings ratio) of N/A.
About Achillion Pharmaceuticals Inc (NASDAQ: ACHN)Achillion Pharmaceuticals, Inc. (Achillion) is a biopharmaceutical company focused on the discovery, development and commercialization of treatments for infectious diseases. Within the anti-infective market, the Company focuses on the development of antivirals for the treatment of chronic hepatitis C and the development of antibacterials for the treatment of resistant bacterial infections. As of December 31, 2009, Achillion focused on developing three Hepatitis C
virus (HCV) drug candidates: ACH-1625, a protease inhibitor for the treatment of chronic hepatitis C in phase Ib clinical testing; ACH-1095, a NS4A antagonist also for the treatment of chronic hepatitis C, in late stage preclinical testing, and ACH-2684, a high-potency protease inhibitor in preclinical testing. In addition, it has established other product candidates, which include ACH-702 for the treatment of serious bacterial infections and elvucitabine for the treatment of human immunodeficiency virus (HIV) infection.
For more information about
Zacks Investment Research‘s equity research offerings, visit
Zacks.com.
..,
“There has been no systemic change in how the FDA is approaching drug approvals” Walsh said in an e-mail. “The primary factor driving first-cycle approval is the quality of the application.”No drugmaker had more than one new medicine approved in 2010, according to data Bloomberg compiled. The figures, derived from an agency database of “new molecular entities,” exclude blood products and vaccines such as Seattle-based Dendreon Corp.’s Provenge for prostate cancer, approved April 29 after a three-year wait, because the FDA doesn’t consider them drugs.
Merck, of Whitehouse Station, N.J., made progress in 2010 launching new products and advancing its drug pipeline, said Ron Rogers, a spokesman. Products to be evaluated this year include boceprevir, a hepatitis C treatment that five analysts project, on average, will have sales of $524.4 million in 2014.
.
Dynavax Technologies Corporation (Dynavax) is a biopharmaceutical company that discovers and develops products to prevent and treat infectious diseases, asthma and inflammatory and autoimmune diseases. The Company’s principal product candidate is HEPLISAV, a Phase III investigational adult hepatitis B vaccine. Its pipeline of product candidate includes HEPLISAV; its Universal Flu vaccine; clinical-stage programs for hepatitis C and hepatitis B therapies, and preclinical programs partnered with AstraZeneca and GlaxoSmithKline (GSK). In January 2010, the Company announced the completion of the acquisition of Symphony Dynamo, Inc.
Dynavax Technologies Co. (NASDAQ: DVAX) traded down 3.44% during mid-day trading on Monday. The stock has a 52 week low of $1.19 and a 52 week high of $3.24. Its 50-day moving average is $2.38 and its 200-day moving average is $2.01. The company has a market cap of $357.1 million and a price-to-earnings ratio of N/A.
Stay on top of analysts' coverage with American Banking & Market News' daily email newsletter that provides a concise list of analysts’ upgrades, analysts’ downgrades and analysts’ price target changes for each day. Click Here to register..
..
Dec 2010
.
This is supposed to be Cambridge-based
Vertex Pharmaceuticals’ big year. The company has been steadily adding staff over the past year and a half, as the company gears up for its anticipated transformation to a profitable, commercial biopharmaceutical company, joining the elite ranks of its neighbors
Biogen Idec and
Genzyme Corp.Vertex submitted its much-anticipated drug candidate Telaprevir, for the treatment of hepatitis C to the U.S. Food and Drug Administration in November. Vertex has asked for a priority review, meaning that a decision could come as soon as May.
“This submission is a milestone in our more than 15-year effort to change the way hepatitis C is treated,” said Matthew Emmens, chairman, president and CEO of Vertex, at the time. But the company has recently halted two other, earlier stage clinical trials testing Telaprevir in conjunction with its other potential hepatitis C therapy called VX-222, because the combination wasn’t working. Three other trials, using Telaprevir in combination with other, non-Vertex drugs, are ongoing.
The stakes are high. Howard Liang, an analyst at Boston-based investment bank Leerink Swann has estimated that telaprevir may generate $2.6 billion annually by 2013, if approved. While its partners, Belgium-based Tibotec Pharmaceuticals and Japan-based Mitsubishi Tanabe Pharma hold the rights to commercialize the drug outside the United States, it is the American market that is expected to be the biggest revenue driver for Telapre ...
This is supposed to be Cambridge-based
Vertex Pharmaceuticals’ big year. The company has been steadily adding staff over the past year and a half, as the company gears up for its anticipated transformation to a profitable, commercial biopharmaceutical company, joining the elite ranks of its neighbors
Biogen Idec and
Genzyme Corp.Vertex submitted its much-anticipated drug candidate Telaprevir, for the treatment of hepatitis C to the U.S. Food and Drug Administration in November. Vertex has asked for a priority review, meaning that a decision could come as soon as May.
“This submission is a milestone in our more than 15-year effort to change the way hepatitis C is treated,” said Matthew Emmens, chairman, president and CEO of Vertex, at the time. But the company has recently halted two other, earlier stage clinical trials testing Telaprevir in conjunction with its other potential hepatitis C therapy called VX-222, because the combination wasn’t working. Three other trials, using Telaprevir in combination with other, non-Vertex drugs, are ongoing.
The stakes are high. Howard Liang, an analyst at Boston-based investment bank Leerink Swann has estimated that telaprevir may generate $2.6 billion annually by 2013, if approved. While its partners, Belgium-based Tibotec Pharmaceuticals and Japan-based Mitsubishi Tanabe Pharma hold the rights to commercialize the drug outside the United States, it is the American market that is expected to be the biggest revenue driver for Telaprevir.
A blockbuster drug approval in 2011 would also raise the profile of Vertex as an attractive acquisition target, analysts say, as big pharma companies seek to boost their supplies of new approved drugs to replace those that are going off patent.
Julie M. Donnelly can be reached at juliedonnelly@bizjournals.com.
Read Full Article,
Dec 31
At the other extreme, Vertex Pharmaceuticals' (Nasdaq:
VRTX) hepatitis C treatment, telaprevir, seems like a shoo-in. Given the extensive data and unmet need -- current treatments only cure about half of patients -- an approval seems all but certain.
Keeping in mind that you still have to expect the unexpected, of course.
Keep up with the drugs facing FDA decisions using The Fool's
My Watchlist feature or subscribe to Brian Orelli's RSS feed
here.
. ,
Vertex Pharmaceuticals (NASDAQ: VRTX) Given “Neutral” Rating by Zacks Investment Research Analysts
December 31st, 2010 • Equities research analysts at
Zacks Investment Research reiterated a “neutral” rating on shares of Vertex Pharmaceuticals (NASDAQ: VRTX) in a research note to clients and investors on Monday.
Separately, analysts at Canaccord Genuity raised their price target on shares of Vertex Pharmaceuticals to $35.00 in a research note to investors on Tuesday, December 21st. They now have a “hold” rating on the stock.
Vertex Pharmaceuticals Incorporated (Vertex) is engaged in the business of discovering, developing and commercializing small molecule drugs for the treatment of serious diseases. Telaprevir, the Company’s lead drug candidate, is an oral hepatitis C protease inhibitor and a new class of antiviral treatments in clinical development that target hepatitis C virus (HCV), infection. Telaprevir is being evaluated in a registration program focused on treatment-naïve and treatment-failure patients with genotype 1 HCV infection. VX-770, the lead drug candidate in its cystic fibrosis (CF), program is being evaluated in a registration program that focuses on patients with CF who have the G551D mutation in the gene responsible for CF. Vertex is conducting a number of Phase IIa clinical trials of its earlier-stage drug candidates. On March 12, 2009, Vertex acquired ViroChem Pharma Inc. (ViroChem).
Shares of Vertex Pharmaceuticals (NASDAQ: VRTX) traded down 0.79% during mid-day trading on Friday, hitting $35.06. Vertex Pharmaceuticals has a 52 week low of $31.25 and a 52 week high of $44.24. The stock’s 50-day moving average is $34.28 and its 200-day moving average is $34.94. On average, analysts predict that Vertex Pharmaceuticals will post $-0.90
.
Written by Matthew Tindall
Friday, 31 December 2010 08:22
Anadys Pharmaceuticals, Inc.
(Public,NASDAQ:ANDS) increased 2.07%, to close at $1.48 and its overall traded volume was 702,093.00 shares during the last session against its average volume of 882,279.00. ANDS opened the day at $1.55, it made an intraday low of $1.46 and an intraday high of $1.55. The stock has a 52 week low of $0.90 and 52 week high of $3.24. ANDS's market capitalization is 84.51M and it has 57.10M outstanding shares.
About Anadys Pharmaceuticals, Inc. (Public,NASDAQ:ANDS)
Anadys Pharmaceuticals, Inc. is a biopharmaceutical company engaged in developing medicines for the treatment of hepatitis C. The Company is developing ANA598, a small-molecule, non-nucleoside inhibitor of the NS5B polymerase for the treatment of hepatitis C. It has also investigated ANA773, an oral, small-molecule inducer of endogenous interferons that acts via the Toll-like receptor 7 (TLR7), pathway in a Phase I trial in hepatitis C. In June 2009, the Company initiated a strategic restructuring to focus its operations on the development of ANA598, in particular the Phase II study of ANA598 in combination with pegylated interferon and ribavirin. As part of the restructuring, it suspended further development of ANA773
Continue reading......
Vertex Pharmaceuticals Incorporated
(Public,NASDAQ:VRTX) decreased -0.37%, to close at $35.34 and its overall traded volume was 630,062.00 shares during the last session against its average volume of 1.78M. VRTX opened the day at $35.39, it made an intraday low of $35.22 and an intraday high of $35.49. The stock has a 52 week low of $31.25 and 52 week high of $44.24. VRTX's market capitalization is 7.18B and it has 203.19M outstanding shares.
About Vertex Pharmaceuticals Incorporated (Public,NASDAQ:VRTX)
Vertex Pharmaceuticals Incorporated (Vertex) is engaged in the business of discovering, developing and commercializing small molecule drugs for the treatment of serious diseases. Telaprevir, the Company’s lead drug candidate, is an oral hepatitis C protease inhibitor and a new class of antiviral treatments in clinical development that target hepatitis C virus (HCV), infection. Telaprevir is being evaluated in a registration program focused on treatment-naïve and treatment-failure patients with genotype 1 HCV infection. VX-770, the lead drug candidate in its cystic fibrosis (CF), program is being evaluated in a registration program that focuses on patients with CF who have the G551D mutation in the gene responsible for CF. Vertex is conducting a number of Phase IIa clinical trials of its earlier-stage drug candidates. On March 12, 2009, Vertex acquired ViroChem Pharma Inc. (ViroChem).
.
ACH-1625 has already been shown to significantly reduce viral loads in patients by 3 to 4.25 log10 and maintain a sustained viral response even after therapy has stopped. It has also been shown to be safe up to 2000mg/day, a level far above the highest dose tested in this Phase IIa.
Pre-clinical studies show ACH-1625 to be additive-synergistic to ribavirin and peg-interferon alpha; this study will be a first look at how well those studies translate in the clinic. Although 28 days is still short, the multiple active drug doses as well as a placebo control will allow investigators to gauge in detail the effectiveness of ACH-1625 in this combination. In any case, a full profile of the compound and its potential as part of this three-drug regimen will be in known by the end of 2011. There’s a lot riding on this study.
Aside from its lead compound, Achillion also has a lineup of several other HCV antivirals in development. The once promising ACH-1095, an inhibitor of the NS4A protease is in Phase I. It was originally developed in collaboration with Gilead (
GILD), but its rights have since been handed back to the company- though Gilead still retains the ability to opt in at a later stage in the compound’s development.
Debrianna Obara, VP, media, Razorfish Health
In the digital world of health, more and more brands will focus on distribution of content as opposed to straight display media or search buys. This shift will allow brands who have invested in educational and branded content to amortize that investment by
getting more health seekers to interact with that content. The user benefits, as they can interact with valuable information without leaving their trusted 3rd party website of choice (such as AOL/Yahoo!/WebMD).
By contrast, growth of just 1% to 3% is forecast for the major European markets and Canada, with 3% to 5% growth predicted in the United States, which is still the world's largest drug consumer with 2011 sales expected to hit $320-$330 billion, up from $310 billion this year.
A tougher regulatory environment in the developed countries. The U.S. Food & Drug Administration and many foreign regulatory bodies are becoming more reluctant to grant initial approval for new drugs in the face of numerous recalls and growing safety concerns among the public.
Pressure from governments and private insurers to reduce medical and drug costs. Governments in virtually all of the developed countries are pushing cost-cutting measures, including increased use of generic medications, mandatory price cuts for brand-name drugs and elimination of rebates. Private insurers are increasing requirements for pre-authorization of treatments and higher cost-sharing percentages for patients.
Three Upcoming Make-or-Break Biotech Approvals
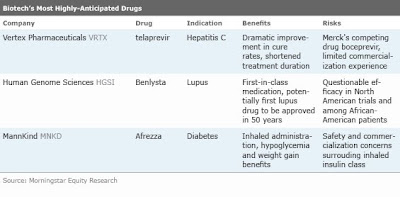 Vertex's Telaprevir Aims to Revolutionize HCV Treatment
Vertex's Telaprevir Aims to Revolutionize HCV Treatment
Vertex (
VRTX) is close to commercializing its hepatitis C drug telaprevir, part of a new class of therapies that have the potential to revolutionize the way the disease is treated. HCV's current standard of care requires 48 weeks of treatment, causes terrible side effects, and is still only able to cure patients 50% of the time. In contrast, telaprevir has the potential to cut treatment time in half and double cure rates. The drug is widely regarded as a major advancement, and we think telaprevir could hit the market in the first half of next year.


 Vertex's Telaprevir Aims to Revolutionize HCV Treatment
Vertex's Telaprevir Aims to Revolutionize HCV Treatment